That itchy, red rash that appears every time you wear your favorite watch or use a new shampoo isn’t just bad luck. It’s likely contact dermatitis, specifically the allergic type known as allergic contact dermatitis (ACD). This condition is a delayed immune reaction where your skin turns against specific chemicals it touches. Unlike an immediate food allergy, this flare-up can take days to show up, making it tricky to pin down the culprit.
If you’ve been dealing with unexplained rashes for months or even years, you’re not alone. Millions of people struggle with this every year, often trying countless creams that only treat the symptoms, not the cause. The real solution lies in identifying exactly what triggers your skin and learning how to avoid it effectively. Here is how you can get to the bottom of your skin issues and finally find relief.
Understanding the Trigger: What Causes Allergic Contact Dermatitis?
To stop the itching, you first need to understand what’s happening under your skin. Allergic contact dermatitis is a delayed-type hypersensitivity reaction. It doesn’t happen instantly. Instead, tiny chemicals called haptens penetrate your skin barrier. These haptens bind to proteins in your body, tricking your immune system into thinking they are invaders. Your Langerhans cells pick them up and send signals to your T-cells, launching an inflammatory attack that results in redness, swelling, and intense itching.
This process explains why the rash might appear on parts of your body far from where you touched the allergen. For example, touching a nickel button on your jeans might cause a rash on your neck if you scratch your face afterward. Common culprits include:
- Nickel: Found in jewelry, belt buckles, and phone cases. It affects nearly 15% of people tested.
- Fragrances: Hidden in soaps, lotions, and detergents. Affects about 1-4% of the general population.
- Cobalt: Often found alongside nickel in metals and some cosmetics.
- Balsam of Peru: A resin used in flavorings and perfumes.
- Preservatives: Like thimerosal or formaldehyde releasers in personal care products.
Knowing these common triggers helps you start suspecting certain products, but guessing is dangerous. You need concrete proof to know what to avoid safely.
The Gold Standard: Patch Testing Explained
You cannot reliably identify contact allergens by looking at product labels alone. Many ingredients have hidden names or cross-contaminants. The most reliable way to diagnose ACD is through patch testing, which is considered the gold standard diagnostic method by dermatologists worldwide.
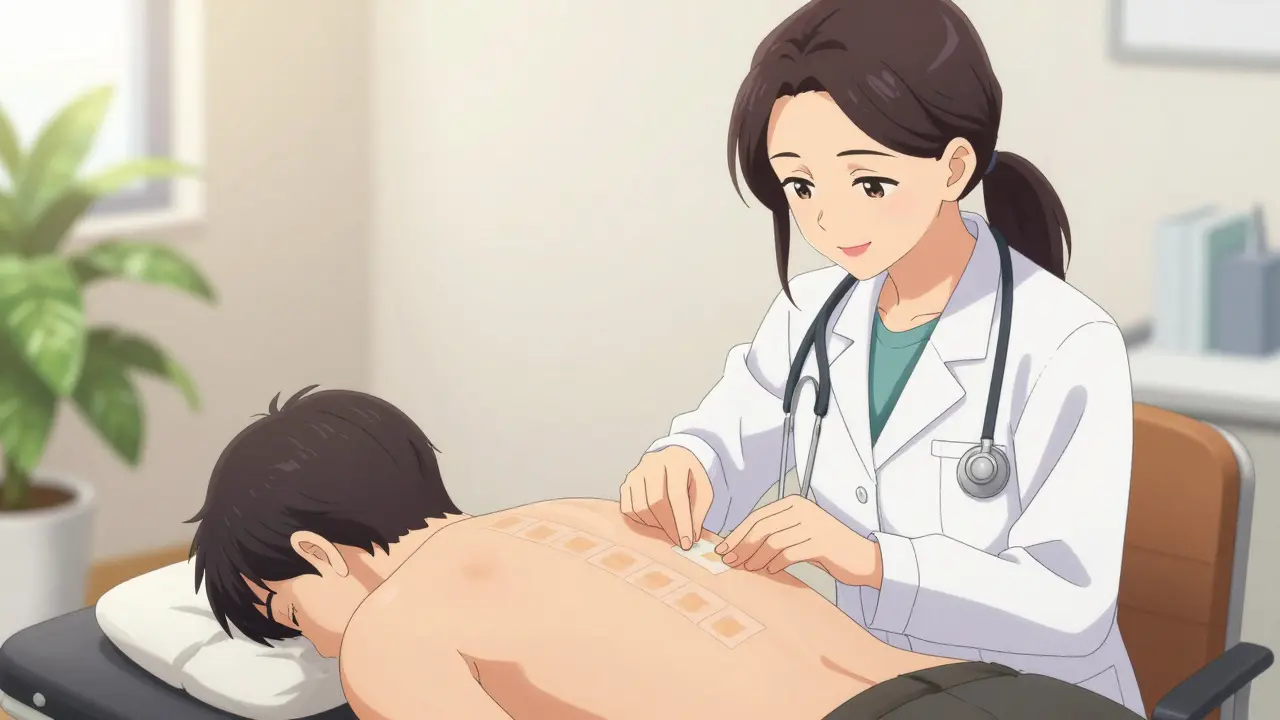
Unlike skin prick tests used for pollen or pet allergies, patch testing checks for those slow-burning reactions. During the procedure, small patches containing potential allergens are taped to your back. You typically leave them on for 48 hours. Then, you return to your doctor for readings-usually at 48 hours and again at 96 hours. This timeline ensures you catch any delayed reactions.
The standard test, often called the TRUE Test, includes 29 common antigens. If you react to one, your skin will show a distinct bump or blister at that specific spot. However, there are thousands of potential allergens. If the standard panel comes back negative but you still have symptoms, your doctor might recommend an expanded series, testing up to 70-100 substances, especially if you work in high-risk fields like healthcare or construction.
| Method | Best For | Timeframe | Limitations |
|---|---|---|---|
| Patch Testing | Delayed reactions (ACD) | 48-96 hours | Only tests specific panels; requires expertise to read |
| Skin Prick Test | Immediate reactions (pollen, pets) | 15-20 minutes | Ineffective for contact dermatitis |
| Blood Tests (IgE) | Systemic allergies | Days for results | Does not detect contact sensitizers |
Interpreting Results and False Negatives
Getting your patch test results is a big step, but it’s not always straightforward. Studies show that interpretation can vary between doctors, with up to 30% variability among non-specialists. This is why seeing a contact dermatitis specialist is crucial. They look for true positive reactions while ruling out irritant responses, which can look similar but aren’t allergies.
A major concern for patients is false negatives. About 33% of patients may need expanded testing because the standard 29-allergen panel misses less common triggers. For instance, if you’re allergic to a specific preservative in hair dye that isn’t on the standard list, the initial test won’t catch it. If your standard test is negative but your rash persists, ask your doctor about expanded series testing or bringing in your own suspected products for testing.
Conversely, false positives can occur if you scratch the patches or get sweat underneath them. That’s why following the preparation instructions-like avoiding showering heavily or sweating excessively during the test-is vital for accurate results.
Creating an Effective Avoidance Strategy
Once you know your allergens, the next challenge is avoiding them. This is often harder than people expect because allergens hide in plain sight. Nickel, for example, leaches from metal objects when they touch sweaty skin. Fragrance mixes can contain dozens of individual scent compounds, any of which could trigger a reaction.
Here is a practical approach to building your avoidance plan:
- Read Labels Rigorously: Learn the chemical names of your allergens. Fragrance might be listed as "parfum," "aroma," or specific botanical extracts.
- Use Barrier Protection: For occupational exposures, gloves and protective clothing can prevent direct contact. Ensure the gloves themselves don’t contain latex or accelerators you’re also allergic to.
- Switch Products Gradually: Replace shampoos, soaps, and lotions with hypoallergenic alternatives. Look for brands certified by organizations like the National Eczema Association.
- Check Household Items: Laundry detergents and fabric softeners are common sources of residual allergens on clothes.
Resources like the Contact Allergen Replacement Database (CARD) can help you find safe alternatives for over 18,000 consumer products. Using such tools reduces the guesswork and helps you maintain a normal routine without triggering flare-ups.

Occupational Risks and Workplace Safety
If your job involves frequent hand washing, chemical exposure, or wearing protective gear, you are at higher risk. Occupational contact dermatitis accounts for nearly 20% of all work-related illnesses in some sectors. Hairdressers, healthcare workers, and construction employees face the highest prevalence rates.
In many regions, employers are required to cooperate in identifying workplace allergens. If you develop ACD, document your exposure history and share your patch test results with your occupational health provider. They can help implement controls, such as providing allergen-free gloves or adjusting tasks to minimize skin contact. Remember, early intervention prevents chronic skin damage that can become permanent even after removing the allergen.
Future Innovations in Diagnosis
While patch testing remains the clinical standard, science is moving forward. Researchers are exploring molecular biomarkers, such as IL-18 blood levels, which correlate with disease severity. In the future, we might see non-invasive blood tests that complement traditional patch testing, offering faster and more objective diagnoses. Additionally, regulatory bodies are pushing for stricter limits on known sensitizers, particularly in the European Union, which has banned or restricted over 26 fragrance allergens in cosmetics. These changes aim to reduce the overall burden of contact dermatitis globally.
Until then, the best defense is knowledge. By identifying your specific triggers through proper testing and diligently avoiding them, you can significantly reduce symptoms and improve your quality of life. Don’t let a mystery rash dictate your daily choices-take control with accurate diagnosis.
How long does patch testing take?
Patch testing typically spans 96 hours. You apply the patches, leave them on for 48 hours, and then return for readings at 48 and 96 hours. This usually involves three clinic visits, often scheduled on Monday, Wednesday, and Friday.
Can I shower during patch testing?
You should avoid heavy sweating and excessive water exposure. Light washing of areas away from the back is usually okay, but soaking the patches can cause them to fall off or create false reactions due to moisture irritation.
What if my patch test is negative but I still have a rash?
A negative result means the common allergens weren’t detected. You may need an expanded series testing more rare substances, or your rash might be caused by an irritant rather than an allergy. Consult your dermatologist for further investigation.
Is nickel allergy common?
Yes, nickel is the most prevalent contact allergen globally. It affects approximately 14-17% of women and about 3% of men in North America, often triggered by jewelry, belts, and electronics.
Does avoiding allergens cure contact dermatitis?
Avoidance is the primary treatment. While it doesn't "cure" the underlying sensitivity, strict avoidance typically leads to significant symptom improvement, with 82% of patients reporting better outcomes after implementing targeted avoidance strategies.
